From Sales Floors to Sore Feet: A Physiotherapist’s Guide to Pain-Free Standing
Are you a sales professional spending long hours on your feet, greeting clients with a smile while dealing with aching feet, tired legs, or back pain by the end of the day?
You’re not alone! As a physiotherapist, I see this every week. The good news is that small changes can make a big difference.
Understanding Musculoskeletal Problems from Prolonged Standing
When you stand for hours, your muscles and joints are under constant load with reduced circulation. Over time, this can lead to fatigue, tightness, and pain, particularly in the lower back, knees, legs, and feet.
Does this sound like you?
Aching or stiffness in the lower back that builds up as the day goes on
Heavy, tired legs, sometimes with mild swelling around the ankles
Discomfort around the knees, especially near the kneecap
Heel pain or sharp discomfort under the foot, particularly first thing in the morning
Tight calves or a pulling sensation in the Achilles tendon
General foot fatigue or aching arches
These issues often start gradually but can become more persistent if left unaddressed.
The Big Why - The Biomechanics
In good standing posture, your body’s weight is balanced through your joints so that muscles and ligaments share the load comfortably. However, when standing still for long periods, small changes begin to occur:
Your body isn’t designed to stay in one position. Muscles become tired and your joints start taking more strain than they should.
Blood flow in the legs can slow down, causing heaviness or swelling.
The natural curve in your lower back may flatten or become overly arched.
Knees often lock backwards, placing extra pressure on the joint surfaces.
Feet tend to roll inwards, flattening the arches and straining the tissues on the bottom of the foot.
These subtle shifts add up, creating stress that can lead to pain and reduced comfort.
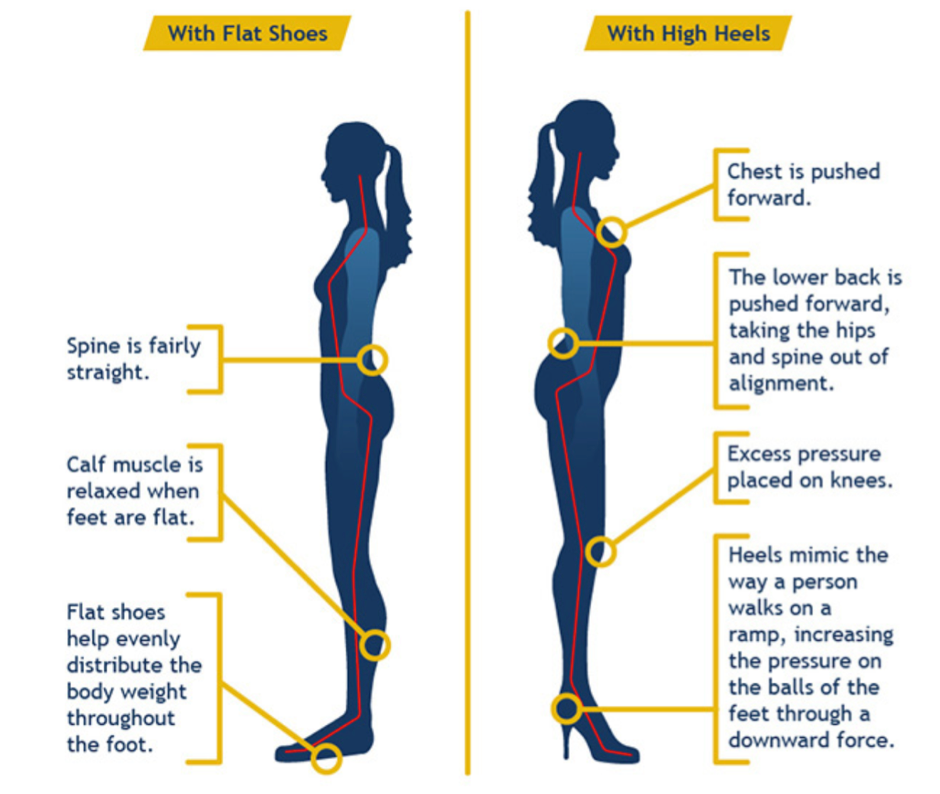
How High Heels Change the Picture
Stylish heels may be part of your professional look; however, they can also change the way your body aligns from the ground:
The heel shifts your weight forward onto the balls of the feet, increasing pressure in the forefoot.
Your pelvis tilts forward and the lower back arches more, which can compress the joints in the spine.
The calf muscles and Achilles tendon remain shortened throughout the day, leading to tightness and reduced flexibility.
This altered posture places additional strain on the knees and lower back.
What You Can Do About It? – Practical Steps That Help
The good news is that small, consistent changes can make a real difference. Here’s what I often recommend to clients in similar situations:
Smart Footwear Choices: Go for shoes with a low, stable heel (ideally no more than 3–4 cm) and good arch support whenever possible. Many of my clients keep a comfortable pair of supportive flats or cushioned shoes at work to alternate with heels during quieter moments.
Movement and Posture Habits
Keep your knees softly unlocked rather than locked back.
Shift your weight gently from side to side or heel to toe every few minutes.
Use a low footrest to rest one foot on, alternating sides regularly.
Set a gentle reminder every 30–45 minutes to reset your posture with a neutral spine.
Daily Stretches and Strengthening: Try these simple exercises:
Calf Stretch: Stand facing a wall with one foot back and heel on the ground. Hold for 30 seconds on each side.
Hip Flexor Stretch: Step one foot forward into a gentle lunge and ease your hips forward. Hold 30 seconds per side.
Glute Bridge: Lie on your back, feet flat, lift your hips while squeezing your glutes. Do 12–15 repetitions.
Foot Doming: While seated or standing, gently lift the arch of your foot without curling your toes. Repeat 10–15 times per foot.
End-of-Day Recovery: Apply ice to sore areas for 15–20 minutes and elevate your legs when you get home. Compression socks can also help reduce heaviness and swelling after long shifts.
When to Seek Professional Help
If the discomfort is becoming more frequent, affecting your sleep, or not improving with these changes, it’s worth having a proper assessment. In the clinic, I do a detailed postural and movement analysis to find out what’s contributing to your symptoms. Treatment includes manual therapy, dry needling, targeted exercises, or advice on orthotics if needed.
A helpful tip I often share: Even if your shoes still look good, replace them when the internal cushioning starts to break down – usually every 6–12 months depending on how much you stand.
Final Thoughts
Prolonged standing doesn’t have to mean living with daily discomfort. By understanding how your body responds to long hours on your feet and making a few adjustments, you can feel noticeably better.
If you would like a personalised assessment or a tailored plan to suit your specific role and symptoms, I would be happy to see you in the clinic. Many of my clients in luxury retail tell me they wish they had sought help sooner.
Wishing you comfort and confidence on your feet.
Ready to Start Your Journey? Book A Physiotherapy Session With Nicole Today!
Reaching out to a physiotherapist can be the turning point in your recovery. We're here to help you get back to doing the things you love, without being held back by pain.